Enhance revenue cycle outcomes with machine learning and AI-driven, real-time visibility.
Healthcare organizations are staring down rising denial rates, workforce strain, tighter margins, and accelerating payer complexity. Traditional, reactive denial management can’t keep pace. The organizations winning today aren’t managing denials—they’re preventing them with Predictive Intelligence.
What Is Predictive Intelligence in Revenue Cycle?
Predictive Intelligence uses machine learning to analyze your historical claims and remittance data to:
-
Identify denial patterns
-
Forecast denial risk before submission
-
Highlight root causes
-
Trigger corrective action automatically
Instead of reacting weeks later to a payer rejection, your team fixes the problem before the claim leaves your system. That’s the difference between denial management and denial avoidance. Predictive Intelligence shifts your RCM strategy from reactive to proactive by protecting cash flow and reducing preventable write-offs.
What Predictive Intelligence Actually Does
Here’s how Predictive Intelligence by Quadax (PIQ) transforms daily claims workflow:
🚩Predict Denials Before Claim Submission: Every claim is scored for denial risk. High-risk claims are flagged with clear, actionable reasons.
❌Prevent Errors Upstream: Claims can be automatically halted so teams can correct:
Coding inconsistencies
Demographic errors
Missing authorizations
Documentation gaps
Non-covered services
🔝Prioritize High-Value Claims: PIQ forecasts expected reimbursement and likely days-to-pay so your staff can focus on the claims with the greatest financial impact.
📈Project Cash Flow More Accurately: By gaining more visibility into future payment timing, expected reimbursement yield and denial risk trends.
👥Train Staff in Real Time: Because PIQ explains the “why” behind every prediction, it becomes a built-in training tool that reduces variation and accelerates onboarding.
CASE STUDY: The Power of Predictive Intelligence
How PIQ Provided a 30x ROI in just 60 Days
Crisp Regional Health Services aimed to reduce denials tied to coding and non‑covered services. PIQ analyzed historical patterns, tuned models to Crisp’s data, and implemented automated rules to hold at‑risk claims. And, PIQ flagged patterns within targeted denial codes and enabled corrections before submission.
Validated outcomes: 30× ROI, 125% increase in reimbursement, 60% reduction in targeted denial codes, $93,000+ recovered from prior write‑offs, and a significant reduction in manual touches per claim.
The Results?
-
📈 125% increase in reimbursement
-
📉 60% reduction in denial codes 182 and 96
-
💰 $120,000+ ROI in just two months
-
🔁 $93,000+ recovered from previously written-off claims
-
⏱ Significant reduction in manual touches per claim
“The integration of (Quadax's) Predictive Intelligence tool surpassed my expectations by effectively demonstrating its ability to exceed our reimbursement goals.”
— Crisp Regional Hospital, Medical Billing Manager
Crisp didn’t just reduce denials. They recovered revenue they thought was gone.
🔗Download the PIQ Research Report
Why Predictive Intelligence by Quadax Is Different
-
Not a bolt‑on—built into the work. PIQ lives inside claims and remittance workflows where decisions happen, not in a separate dashboard that staff has to check later.
-
Your data builds the model. PIQ trains on your historical claims and payer behavior to deliver accurate, explainable predictions specific to your mix.
-
Action in the flow, not after the fact. High‑risk claims are automatically halted with guided corrections; recurring patterns convert to configurable rules that scale prevention.
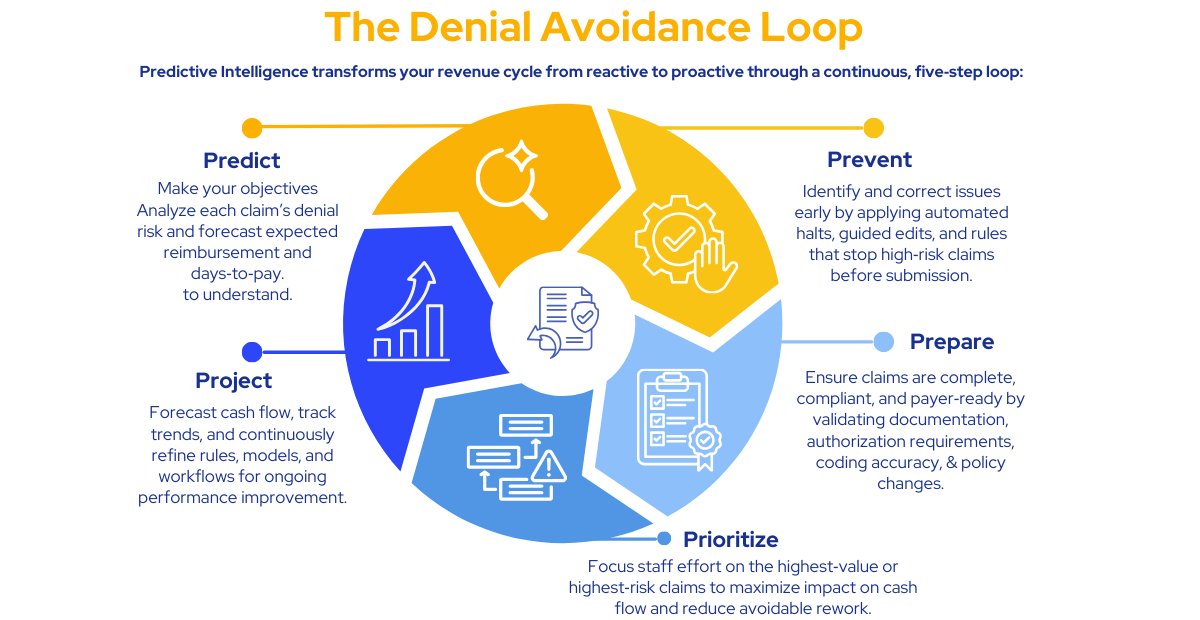
What Revenue Cycle Leaders Can Expect
For CFOs, revenue cycle directors, and patient financial services leaders, Predictive Intelligence delivers measurable impact:
Revenue Protection: Fewer preventable denials = stronger margins.
Improved Cash Flow Visibility: Forecasted payment timelines improve planning accuracy.
Labor Efficiency: Reduced rework means fewer manual touches and less burnout.
Reduced Payer Risk: Stay ahead of evolving documentation requirements and payer automation
Faster Time-to-Value: Most organizations see measurable financial impact within 60–90 days.
See What PIQ Would Find In Your Data
Don’t guess. Let your numbers show where revenue is leaking.
Click here to schedule a personalized denial analysis with us today.
Predictive Intelligence in revenue cycle management isn’t just an upgrade. It’s a competitive advantage, and it’s transforming how healthcare organizations get paid.


